“You’re just tired,” Simmons said. “You’re tired of checking your blood a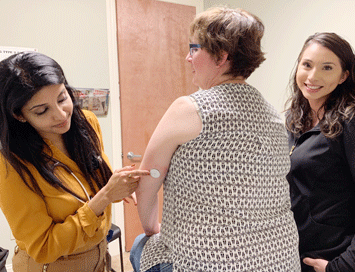 nd you need to because if you plan on living a long life you need to keep your blood sugar within certain ranges.”
nd you need to because if you plan on living a long life you need to keep your blood sugar within certain ranges.”
So when UCSF Fresno’s Varsha Babu, MD, suggested Simmons try a continuous glucose monitor that would allow her to control her diabetes without painful fingersticks, Simmons quickly agreed.
“This does not hurt,” Simmons said as she demonstrated how she now can check her blood glucose by swiping her cellphone over a sensor about the size of a coat button placed on her upper left arm.
Babu, an endocrinologist, said a fingerstick can be more painful than an insulin shot because the gauge that pricks the finger is thicker than an insulin needle. “So my patients are willing to do the shots but they are not willing to test their blood sugar,” she said.
Checking blood glucose levels is essential to good diabetes management. Multiple studies show the more testing, the better control. And for the past year, Babu and fellow UCSF Fresno endocrinologists have been placing continuous glucose monitors on patients with Type 1 and Type 2 diabetes, with good results. Both Type 1 and Type 2 diabetes affect the way the body regulates blood glucose, but patients with Type 1 diabetes do not produce insulin, a hormone that takes glucose and uses it for energy. Patients with Type 2 diabetes either do not make enough insulin or they have insulin resistance and require higher levels of insulin to bring down blood sugars to normal ranges.
The monitors eliminate painful finger pricks and the social stigma of checking blood glucose in restaurants or other public places, Babu said.
Babu and her fellow UCSF Fresno endocrinologists have started diabetes education clinics for patients with the new monitors and those with insulin pumps (a medical device that administers insulin through a catheter under the skin). “We have dietitians available and highly trained medical assistants,” Babu said. “We are really trying to promote more care for our Valley.”
Diabetes patients in the San Joaquin Valley can benefit more than most from new technology and education. Kern County has the highest age-adjusted death rate for diabetes, according to the California Department of Public Health. Kern County’s death rate is 36.1 deaths per 100,000 population compared to a statewide rate of 20.7. The counties of Fresno, Madera, Merced, Tulare, Kings, Stanislaus and San Joaquin also have diabetes death rates higher than the state average and among the highest in the state.
Babu has seen improved hemoglobin A1c levels in Type 2 patients who have struggled to control their diabetes. A1c tests show average blood glucose levels and some patients have had significant drops — from higher than 10 percent to less than 7 percent. (An A1c level below 5.7 percent is considered normal).
Patients say the monitors are life changers, said Maria Barajas, a medical assistant at University Diabetes and Endocrine Specialists, one of the many UCSF faculty physician offices in Fresno that are part of the University Centers of Excellence. “Some of the patients are needle phobic. They hate pricking their fingers or they work in offices where they can’t be pricking their fingers.”
Simmons, a high school teacher, has Type 2 diabetes that she controls with oral medications, diet and exercise. It was not practical to prick a finger in a classroom but a Freestyle Libre 14 Day monitor lets her easily check blood glucose throughout the day. The monitor came with a reader that she carries in her purse but she programmed her cellphone to scan for readings.
Two types of continuous glucose monitors are available – intermittent and real time, Babu said. The monitors’ sensors are similar, but patients who have intermittent sensors, such as the Freestyle Libre 14, scan to get a glucose reading. Real-time monitors, such as the Dexcom G6, display the glucose number without scanning and the monitor can be connected directly to an iPhone or any Apple device. The Dexcom G6 also sounds an alarm when glucose levels are low or high and doctors can set the levels for the alerts. Up to five people can share the data.
The Freestyle Libre Day 14 sensor lasts for two weeks and the Dexcom G6 for 10 days and patients are taught how to replace the sensors. Many insurance plans cover the devices, including Medicare and Medi-Cal, and patients are helped through the process of getting insurance approval.
Sharing technological advances, such as continuous glucose monitors, with patients is part of improving the health of the community, Babu said. “I would like to say that very soon we should have some cure for diabetes – but until that time, this is the best we have so far and it’s proven to be useful.”



.jpg)
.jpg)
.jpg)
.jpg)